-
Address: Suite 4 (level 1), 52 Hatherley Parade, Winthrop, WA 6150.
-
Phone: 08 9332 2455
-
Email: reception@waurology.com.au

Radical Cystectomy And Formation Of Ileal Conduit
Procedure Information
Dr Vasudevan has recommended that you have a radical cystectomy and formation of ileal conduit. This document gives you information on what to expect before, during and after the operation. If there are questions that this document does not answer, please ask Dr Vasudevan.
What Is A Radical Cystectomy?
A radical cystectomy is the removal of the bladder and lymph nodes in the pelvis. In men, the prostate gland and seminal vesicles are also removed. In women, the uterus, ovaries and the top of the vaginal wall may be removed as well.
What Is a An Ileal Conduit?
This is when a section of your small bowel is used as a means of draining urine out of the body when the bladder has been removed.
Why Do I Need A Radical Cystectomy?
You would have had a scraping of a bladder tumour from your bladder (TURBT). The results of the bladder tumour would have shown it to be muscle invasive. Because it is invading into the bladder muscles, the best way to achieve cure is to remove the whole bladder.
Are There Any Alternatives?
It is possible to have what is called a continent urinary diversion, also called neo bladder. If this is done you will need to regularly pass a catheter via your urethra into the neo bladder to drain the urine.
The information in this document will be limited to the ileal conduit.
Radiotherapy is an alternative to a radical cystectomy. If you choose to have this treatment, Dr Vasudevan will refer you to a radiation oncologist.
What Happens In The Pre-Operative Consultation?
Dr Vasudevan will arrange a date for your operation. You would have by now also had CT scans to ensure that the cancer is confined to the bladder. Dr Vasudevan will organise routine blood tests, Chest X-ray and ECG prior to your surgery. He will discuss the operation with you and get you to sign the consent form for the surgery.
Dr Vasudevan, will also refer you to a stoma nurse, who will teach you how to care for your stoma after the operation. The stoma nurse will also mark on your abdomen an appropriate location for the stoma. The stoma is usually on the right side of the abdomen and just below the waist.
What Should I Do About My Medications?
Please inform Dr Vasudevan of all the medications that you are on in the pre-operative consultation. If you are taking some blood thinning medications they may need to be stopped prior to surgery. He can advise you appropriately.
What Can I Do To Make The Operation A Success?
If you smoke, stopping smoking several weeks or more before the operation may reduce your risk of developing complications and will improve your long-term health. Try to maintain a healthy weight. You have a higher risk of developing complications if you are overweight. Regular exercise should help to prepare you for the operation, help you to recover and improve your long-term health.
What Does The Operation Involve?
 In preparation for the surgery you will be instructed to have only clear fluids for 24 hours prior to your surgery. You will need to fast (ie: keep nil by mouth) from midnight the day prior to your surgery.
In preparation for the surgery you will be instructed to have only clear fluids for 24 hours prior to your surgery. You will need to fast (ie: keep nil by mouth) from midnight the day prior to your surgery.
Once you come to the hospital, the healthcare team will carry out a number of checks to make sure you have the operation you came in for. You can help by confirming to Dr Vasudevan and the healthcare team your name and the operation you are having.
You will be given anti-embolic stockings to wear prior to surgery to reduce the risk of blood clots in your legs.
Once in the operating theatre you will be given a general anaesthetic, so that you will not be aware of anything whilst the operation is being performed. The anaesthetist will discuss this with you.
You will be given antibiotics through your veins at the commencement of the operation to minimise any risk of infection.
A cut will be made from your belly button to just above the pubic bone. The bladder is dissected and freed from all its attachments including the ureters (tubes that carry urine from the kidneys to the bladder). Depending on if you are a male or female other organs will be removed as described previously. Lymph nodes in the pelvis are also dissected out.
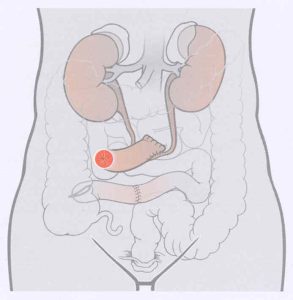
An ileal conduit is formed by isolating a segment of your small bowel called ileum. Once this segment is isolated the two ends of the bowel are re-joined to allow for bowel contents to continue.
Using the isolated segment of ileum (also called conduit), the ureters are stitched into one end of the conduit. Stents are placed in the ureters to allow the join to heal properly. The other end of the conduit is brought out to the pre-marked stoma site. The stents placed in the ureters will come out of the stoma. The urine can then flow from the ureters, through the conduit to the stoma on the abdomen. A bag is placed over the stoma site to collect the urine. A drain tube is placed in the pelvis to drain away any blood or fluid that may accumulate in the pelvis after the operation. The wound is closed with dissolving stiches.
The operation takes about 5 to 6 hours.
What Can I Expect After The Operation Is Completed?
You will wake up in the recovery area in your bed. When the nurses in the recovery area are happy with your condition a nurse from the ward will take you back to the ward.
Depending on how you recover and the complexity of the operation you may require a period of intensive monitoring in the intensive care unit. This decision will be made either in the operating room or in the recovery ward.
Once in the ward you may have a number of attachments which are either monitoring your vital parameters or are assisting with your recovery.
The attachments might include:
Oxygen
Given for a short time till you are more alert
Intravenous fluids
This is given into your veins via a drip to make sure that you do not get dehydrated. The fluids will gradually be removed and replaced with oral fluids and then a normal diet once your bowels have started to work again. You will know that your bowels are working again when you start passing flatus.
Drain tube
This is usually removed after about 2 days. If the drain is still draining a large amount of fluid it will be left in for a longer period of time.
PCA (patient controlled analgesia)
This is where you will be able to administer yourself pain relief as required through your veins. Once you can eat and drink this will be removed and replaced with oral pain killers.
You will be encouraged to get up and about as soon as possible to avoid complications such as clots in the legs. Once you are reasonably independent and can care for the stoma yourself you will be discharged home. On average patients are discharged from about 7 to 10 days after surgery.
What Are The Possible Complications Of A Radical Cystectomy?
Dr Vasudevan will try to make the operation as safe as possible but sometimes complications can happen.
The possible complications include:
Anaesthetic complications
The anaesthetist will discuss this with you.
Bleeding
Excessive blood loss requiring blood transfusion is uncommon. If you do not consent to blood transfusions please let Dr Vasudevan know prior to surgery.
Prolonged ileus
It is common for your bowels to take 4 to 5 days after surgery to function again. The period of time that the bowels do not work is called ileus. If this period is prolonged it may be required to give nutrition fluids called TPN via your veins. This may happen in 12% to 20% of cases.
Pneumonia
This is an infection in your lungs and may arise due to prolonged bed rest. It can occur in 2% of cases.
Leakage from the bowel or ureter join
While this is rare (1%) if it does occur repeat surgery is required.
Deep Vein thrombosis
This is a blood clot in your leg. It is rare (1%). If present it can cause pain, swelling or redness in your leg. If you notice these symptoms please inform Dr Vasudevan and further investigations will be needed and if confirmed will need blood thinning medications.
Pulmonary Embolus
This is a blood clot in the lung and is rare (1%). It gets there when a piece of blood clot breaks off from a clot in the leg and by moving through the blood stream lodges itself in the lung. It can cause shortness of breath and chest pain. If you experience such symptoms when at home please call an ambulance and present to the nearest emergency department.
Infection
Antibiotics are given during the surgery to minimise the chance of infection in the post-operative period. If despite this you notice any symptoms of an infection such as redness to the wound, fever or discharge from the wound please inform Dr Vasudevan. If infection is confirmed antibiotics will be given to treat it.
Hernia
This is where a part of the abdominal contents protrudes through a weak section. The weak section can be at the site of the abdominal incision or around the stoma site. If the hernia is causing symptoms repeat surgery will be needed to repair it. If the hernia is not causing any symptoms you may elect to leave it alone.
Scarring of the join between ureters and bowel
This is may occur in 2% to 5 % of cases. This if undetected may over a period of time cause failure of the kidneys. Hence it does need surgical correction when identified.
How Soon Will I Recover?
Pain control
You will be given pain killers to take home. Use these as directed. If there is excessive pain please inform Dr Vasudevan.
Showering
You may shower as per normal when you return home. The wound sites can get wet, but must be padded dry after showering. Tub baths are not recommended in the first 2 weeks after surgery as this will soak the incision and increase risk of infections
Bowels
You can eat and drink as per normal. On occasions constipation can be a problem and you may need laxatives to help with bowel actions.
Activity
Taking walks is advisable. Prolonged sitting or lying in bed should be avoided. Climbing stairs is allowed but done slowly. Driving should be avoided for 4 to 6 weeks. Do not lift heavy items or do vigorous exercise for 6 to 8 weeks. You can return to work in about 6 to 8 weeks.
Follow-Up Appointment With Dr Vasudevan
Once discharged from hospital please arrange a follow-up appointment with Dr Vasudevan for about 6 weeks after surgery.
During this appointment he will assess your incision and stoma, discuss the result of your bladder and lymph node specimens, remove the stents that are in your ureter, ensure that you are managing to change your stoma bags properly and arrange any further treatment if required.
He will also arrange for subsequent blood tests and scans that are required as part of on-going surveillance.
